The annual incidence of pituitary tumours varies from 2 to 7 cases for every 100,000 people per year. They represent between 10-15% of all intracranial tumours. They are most frequent in women, and appear between the ages of thirty and sixty.
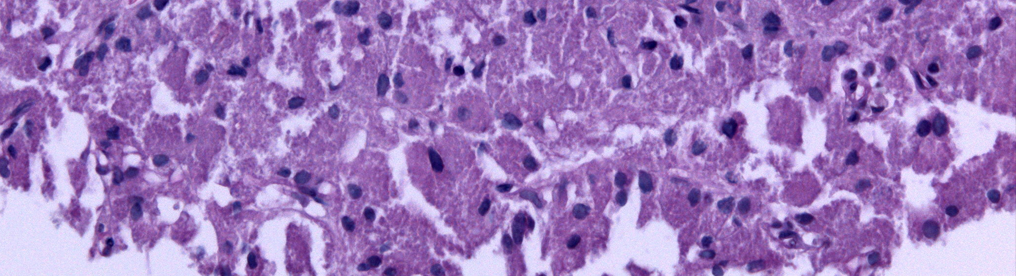
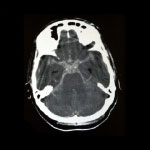
The majority of pituitary tumours are usually benign and have a low growth rate. We generally find the small tumours confined to the sella turcica, although it is not unusual to find the small and medium sized tumours filtering into the cavernous sinus. On the other hand there is the invasive tumour, which follows a more aggressive course. It tends to grow quickly and invade places like the carotid arteries or optic nerves.