SYMPTOMS

Headache
Nausea and/or vomiting
Convulsive seizure
Limb weakness
Uncoordinated gait
Alteration of sensitivity
Double vision or vision disorder
Difficulty with language
Deafness
Paralysis or reduced sensitivity of the face
Difficulty swallowing
DIAGNOSIS
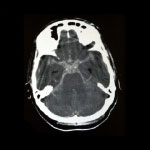
CT SCAN OF THE BRAIN
The brain CT is usually the first test to be carried out. It gives rise to the initial suspicion of a brain tumour because it allows the lesion to be seen, albeit imprecisely.

MAGNETIC RESONANCE IMAGING OF THE BRAIN
La Resonancia Magnética cerebral es la prueba principal y más precisa. Hoy día permite, no solo obtener una imagen muy anatómica del tumor cerebral, sino también estudiar que características tiene. Podemos localizar el tumor, saber su tamaño, si tiene características de más o menos agresividad y si esta en relación con zonas cerebrales que tienen una función importante (sobretodo motora o de lenguaje). Además se suele realizar una secuencia de Resonancia Magnética de alta definición para utilizarla como mapa durante la cirugía y a través de un recurso llamado neuronavegación.
Magnetic resonance imaging of the brain is the primary and most accurate test. Not only does it generate a very anatomical image of the brain tumour, but also enables its characteristics to be studied. We can locate the tumour, determine its size and its aggressiveness, and if it is related to areas of the brain that have an important function (especially motor or language). In addition, a sequence of high-resolution MRI to be used as a map during surgery is usually performed, through a resource called neuronavigation.
WHOLE-BODY PET SCAN
This is used to identify any brain lesions originating in another area of the body, as well as the location of the primary tumour. It is usually used to assess the spread of a cancer if metastasis is suspected.

THORACOABDOMINAL CT SCAN
This is equivalent to a whole-body PET scan but it is somewhat less effective.

BLOOD TEST WITH TUMOUR MARKERS
This blood test is used to complete the study of a cancer with suspected metastasis. Elevated levels of these markers may indicate a primary tumour and its possible location.
TREATMENTS
In most cases, if the brain tumour is not very widespread or the patient's conditions do not allow it, surgery is the main treatment. The role of surgery is twofold: to obtain tissue for accurate tumour diagnosis (biopsy); and to remove as much of the tumour as possible.
Depending on the type of brain tumour, other treatments can be added to make the surgery more radical. These treatments are radiotherapy and chemotherapy. They must be appropriate for the type of tumour in accordance with international protocols. In some cases, such as lymphomas, they may constitute the primary treatment ahead of surgery.
BRAIN TUMOUR SURGERY
In brain tumour surgery, perfect planning is vital. At barnaclínic+, we use the most advanced technological resources to remove the maximum volume of tumour causing the least damage. These resources are: neuronavigation (a system that can locate any brain structure with a high degree of precision), intraoperative MRI (a very useful instrument that shows throughout the operation how much tumour remains to be removed and from which areas), robotic visualisation platform (facilitates better visualisation during surgery and access to complex areas) and neurophysiological monitoring (a resource that helps the surgeon to identify which areas of the brain can be removed and which cannot owing to the important function they perform, primarily movement or language).
The surgery is usually performed under general anaesthesia. In some cases, where it is beneficial to examine language function while the brain tumour is being removed, the patient can be operated on while awake with local anaesthesia. During awake brain surgery, the patient does not feel any pain and is simply asked to cooperate throughout the short procedure of removing a tumour from a location close to the language area. During the rest of the surgery, the patient is deeply sedated.
From a technical perspective, brain tumour surgery consists of making a window in the bone to access the lesion as directly as possible and to avoid causing damage. Using an operating microscope and with very precise removal tools, the brain tumour is gradually removed to the extent that the area and function allow.
When finished, the different layers (meninges, bone, skin) are closed. Drains are sometimes placed under the skin to prevent haematoma.
After the surgery, the patient is moved to the ICU for 24 hours. The following day, if there are no complications, the patient will then be moved to their room to slowly recover for 5 to 6 days.
Following detailed analysis, the diagnosis of the extracted tissue is obtained 7 to 10 days after the surgery. Subsequent treatment will be based on the findings of this diagnosis.
Professionals
Blog b+

Study demonstrates the usefulness of deep brain stimulation for the treatment of schizophrenia and bipolar disorder
An article that has recently been published in the Journal of Psychiatry and Mental Health, [1] in which various barnaclínic+ professionals have participated, has shown that deep brain stimulation, a surgical procedure that involves the placement of a device called a neurostimulator that sends electrical impulses to specific areas of the brain, it can be […]

The neurosurgery operating room incorporates new angiography/CT equipment
The integrated neurosurgery operating room has recently been renovated to continue offering the latest and best technology in intraoperative imaging. In this case, angiography/computed tomography (CT) equipment has been incorporated into the facilities, a new tool that allows for further improvement of both patient safety and the efficiency of interventions and which has been acquired […]
barnaclinic+ incorporates laser ablation for the treatment of brain tumours and epilepsy
In 2021, the Clínic de Barcelona incorporated laser ablation in the treatment of some patients with brain tumours or epilepsy. This technique is now available at barnaclinic+, thus increasing the portfolio of services the centre offers and facilitating patient access to this technology. “Laser ablation is a minimally invasive technique with very good results that […]

