Do you want to request a face-to-face appointment, do you want a second opinion or do you need to be visited but you cannot travel from home or are you in another country? Contact us and we will offer you a solution adapted to your case.
HOW TO PREVENT SKIN CANCER AND MELANOMA?
There is no one hundred percent effective way to prevent skin cancer, but there are a number of measures that can reduce the risk of developing it. In this sense, the best way to prevent melanoma or other skin cancer is to protect the skin from sun exposure or other sources of ultraviolet rays.
· Stay in the shade as much as possible between 10am and 4pm.
· Cover yourself from the sun with clothing, sunglasses and/or sunscreen.
· Avoid artificial tanning methods such as tanning beds or sunlamps.
· Examine your skin regularly and monitor possible changes.
TYPES OF SKIN CANCER
There are different types of skin cancer. The most common skin tumour is basal cell carcinoma, but we can also find squamous cell carcinomas, melanoma or other less frequent skin tumours such as lymphoma or tumours of the glands of the skin, nails or hair.

BASAL CELL CARCINOMA
As we have said, basal cell carcinoma is the most common skin cancer. Usually located in the face, we can also find it in other parts of the body exposed to the sun. It is the most common tumour in women and in people over 50 years of age. Slow growing, it is more common in those who have had cumulative exposure to ultraviolet light. It is a type of skin cancer that has a good prognosis if it is removed in its initial phase and rarely metastasises.

SQUAMOUS CELL CARCINOMA
Squamous cell carcinoma is the second most common type of skin cancer. As in the previous case, it is more common in patients over 50 years of age and accumulated exposure to the sun, however, it usually affects fair-skinned people. Just like basal cell carcinoma, if detected in its early stages, it has a favourable prognosis. This type of tumour can produce metastases in other organs, especially in the lymph nodes.

MALIGNANT MELANOMA
Malignant Melanoma is a type of skin cancer that is caused by an abnormal growth of skin cells called melanocytes. The exact cause of this tumour is unknown, but the appearance of this tumour is attributed to the sun and to the genetic and immune characteristics of the patients. Although it only represents 4% of all skin cancers, it is responsible for 80% of deaths. In recent years, an increase in the incidence of malignant melanoma has been observed. This is attributed to increased sun exposure and the use of artificial tanning methods.

OTHER TYPES OF SKIN CANCER
There are less frequent skin tumours. For example, cutaneous lymphoma, malignant adnexal tumours or connective tissue tumours.
WHO SHOULD HAVE A DIAGNOSIS OF SKIN CANCER OR MELANOMA?
Anyone who has a mole should not think they have skin cancer or melanoma, but if you apply the simple ABCDE rule every morning when showering on your pigmented nevi (mole freckles), you can make a suspected diagnosis and go to your doctor as soon as possible.
ABCDE rule
· A: Asymmetry; the mole is not symmetrical
· B: Borders; the mole does not have blunt edges but are star-shaped.
· C: Colour; if it is the colour of coffee with milk it can be normal, if it is black or blue, or areas of the nevus that have lost colour, suspect Melanoma.
· D: Diameter; if it is less than 6 mm, it is considered normal, if it is bigger than 6 mm, it may be a melanoma.
· E: Evolution; if over time, over a few months, the mole changes its shape, its colour, if it grows or bleeds, suspect melanoma.
WHY CARRY OUT THE DIAGNOSIS OF SKIN CANCER AT BARNACLÍNIC+?

PROFESSIONALS SPECIALISED IN THE DIAGNOSIS AND TREATMENT OF SKIN CANCER INTERNATIONAL REFERENCES
Our team of professionals, led by Dr Susana Puig and Dr Josep Malvehy, has more than 20 years of experience in the diagnosis and treatment of skin cancer, melanoma, skin tumours and dermatological surgery.

THE BEST TECHNOLOGY IN DERMATOLOGICAL DIAGNOSIS
We have the latest technology on the market in dermatological diagnosis and skin cancer. In addition to being able to offer our experience in focal microscopy (an eminently professional-dependent technology), we are one of the only two centres in Spain to have the new Vectra360® robot. It is a state-of-the-art device that combines 3D images and sequential digital dermoscopy images to non-invasively track both melanoma and other types of skin cancer.

REFERENCES IN RESEARCH ON SKIN CANCER
Our specialists lead the IDIBAPS "Melanoma: Imaging, Genetics and Immunology" research group. Thanks to the activity of this research group, the early diagnosis of skin cancer has been improved, limiting the intervention and removal of benign lesions and improving the diagnosis of thin melanomas with a good prognosis. With up to nine lines of research, his work in dermoscopy and genetics and identification of biomarkers for melanoma and non-melanoma skin cancer stand out.
EARLY DIAGNOSIS OF SKIN CANCER AND MELANOMA
Currently the only way to increase the survival rate in Melanoma and skin cancer is early diagnosis and surgery with removal of the primary tumour with wide margins.
Melanoma is classified into different stages from I (one) to IV (four). That is why that patient with a diagnosis of melanoma or skin cancer must be studied exhaustively. A proper diagnosis must be made, a good staging and the most appropriate treatment applied depending on the severity of the disease.
TESTS

DIGITAL DERMATOSCOPY AND BODY MAPPING - VECTRA360®
The Vectra360® is a digital dermodiagnosis robot that allows the best detection of skin cancer. It is a device that combines 3D imaging and sequential digital dermoscopy images for non-invasive tracking of skin lesions. It is equipped with 98 cameras and a cross-polarized illumination system that allows capturing images of the entire surface of the patient's skin. In less than a second, the Vectra360® creates a three-dimensional avatar of the patient, giving specialists a complete, high-definition image of their entire skin.
CONFOCAL MICROSCOPY
Confocal microscopy is a non-invasive diagnostic technique for skin lesions with cell resolution, similar to conventional histology, but in real time and painless. It allows visualising the different layers of the skin and studying its structure, it is used for complex lesions and for the diagnosis of skin cancer when dermoscopy does not offer conclusive results.
TREATMENT OF SKIN CANCER AND MELANOMA
SURGICAL TREATMENT
Treatment of skin cancer usually begins with its surgical removal. The difficulty of skin cancer surgery will depend on the type of tumour, its size and its location. In many cases, the intervention can be performed on an outpatient basis, without the need to be admitted to the hospital. However, sometimes it will be necessary to locate and biopsy or intervene the nodes, in these cases it will be necessary to perform surgery under general anaesthesia. The goal of surgery for skin cancer or melanoma is, in all cases, to eradicate the tumour from the skin, eliminating all possible remains.
NON-SURGICAL TREATMENT
Radiotherapy
Radiotherapy for skin cancer or melanoma works in the same way as for other types of tumours. Through the application of high-energy X-rays, tumour cells are destroyed. It is used both in the tumour and in the affected lymph nodes.
Cryotherapy
Another treatment option for skin cancer is cryotherapy. Before small and superficial skin tumours, through the use of cold, they are frozen and eliminated.
Imiquimod
In some cases of skin cancer, a treatment based on topical preparations can be used.
Photodynamic therapy
As in the case of cryotherapy, another treatment option for superficial skin tumours is photodynamic therapy. With this technique, cancer cells can be selectively burned.
Immunotherapy
In cases of skin cancer or advanced melanoma, which has distant metastases and cannot be treated surgically, immunotherapy may be a treatment option. It uses drugs and/or vaccines that activate the defences against the tumour.
Chemotherapy
Chemotherapy can be especially effective for treating some types of skin tumours. In the case of Melanoma in stages I to IV, surgery can be complemented with chemotherapy, radiotherapy or biological therapy.
Professionals
Our core values are the vocation of patient service and respect for people, and we rely on the intense teamwork and ambition for excellence of our group.
The department consists of a solid team of professionals from various subspecialties and specialised nurses, among others, capable of treating all types of dermatological diseases.
Our renowned and devoted professionals, researchers and educators in the field of Dermatology and Skin Cancer Diagnosis are international leaders.
We are known for providing professional, individualised and compassionate care to all patients.
Blog
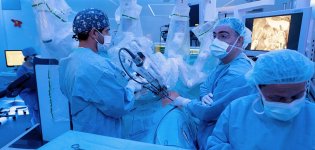
Thoracic Surgery specialists at barnaclínic+ consolidate their international leadership in robotic and minimally invasive surgery
The professionals of Thoracic Surgery at barnaclínic+, all of them members of the Thoracic Surgery Department at Hospital Clínic de Barcelona, continue to consolidate their position as national and international leaders in robotic and minimally invasive thoracic surgery. The robotic surgery program at Hospital Clínic, led by specialists such as Dr. Ricard Ramos, one of […]

International Nurses Day 2026 recognizes nursing talent, innovation and leadership at the Clinic
Under the slogan “Driving Nursing 5.0 Forward Together”, the Hospital Clínic de Barcelona celebrated a new edition of International Nurses Day this May 12, a day focused on recognizing the strategic role of nurses in transforming healthcare systems, advancing clinical innovation, promoting nursing research, and humanizing patient care. The event, held at the Auditorium of […]

visiõnclínic introduces two types of eye exams to improve prevention and control of visual health
visiõnclínic, the ophthalmology clinic of barnaclínic+ and Clínicas Mi, has introduced two new services focused on the control and care of visual health: the Visual Health Pack, with a complete ophthalmological examination, and the Visual Acuity Pack, an eye exam focused on the assessment of visual acuity and prescription check. These new services make it […]


