All therapeutic options for obesity in a single international reference unit
A team with extensive experience in the treatment of obesity with a long history of supporting these patients
When is a medication indicated for obesity?
An obesity medication is indicated in:
· Patients with a BMI ≥30
· Patients with a BMI ≥ 27 if they present obesity-related medical conditions
The indication depends on the class of obesity, cardiovascular risk and the patient’s medical history. The goal is not only weight loss, but also to reduce metabolic, cardiovascular and systemic complications in the medium and long term. Above all, the aim is to improve life expectancy and quality of life.
How do the latest anti-obesity medications work?
New medications for obesity act on hormones that regulate appetite, satiety and energy metabolism.
These anti-obesity medications:
· Reduce hunger.
· Increase satiety after meals.
· Improve insulin sensitivity.
· Promote a sustained reduction in caloric intake.
· May influence metabolic energy expenditure.
They do not replace a healthy lifestyle, but they can be an effective tool within a comprehensive treatment plan supervised by specialists.
Beyond weight loss: metabolic and cardiovascular impact
One of the most relevant aspects of current treatments is that their objective is not solely to lower the number on the scale.
Appetite control and weight reduction are accompanied by:
· Improved insulin sensitivity.
· Lower blood pressure.
· Reduction of inflammatory markers.
· Improvement in lipid profile.
Choosing the right treatment
There is no universal medication suitable for all patients. The choice depends on multiple factors:
· Class of obesity.
· Associated medical conditions.
· Metabolic profile.
· Individual tolerance.
· Therapeutic goals.
For this reason, pharmacological treatment should be initiated within a specialized unit, with structured medical follow-up and gradual dose adjustments.
Main medications currently available for obesity
Pharmacological treatment for obesity has experienced significant advances in recent years. For the first time, we have medications that not only help reduce body weight, but also act directly on the hormonal mechanisms that regulate appetite and metabolism.

Semaglutide (GLP-1 receptor agonist)
Semaglutide belongs to the family of GLP-1 receptor agonists, an intestinal hormone involved in the regulation of appetite and glucose metabolism.
Its mechanism of action is based on:
· Increasing satiety after meals.
· Progressively reducing caloric intake.
· Improving glycemic control in patients with metabolic disorders.
Administered once weekly by subcutaneous injection, it has demonstrated clinically significant weight reduction in clinical trials when integrated into a structured treatment plan. Beyond weight loss, its relevance lies in improving metabolic and cardiovascular profiles.

Tirzepatide (dual GLP-1 and GIP receptor agonist)
Tirzepatide represents an evolution in pharmacological obesity treatment. It acts simultaneously on two hormonal pathways involved in energy balance: the GLP-1 receptor and the GIP receptor.
This dual mechanism allows it to:
· Modulate appetite.
· Optimize metabolic response.
· Promote significant weight reduction in selected patient profiles.
Clinical studies have shown remarkable results in both weight reduction and improvement of metabolic, cardiovascular and other obesity-related conditions. However, its indication must always follow an individualized medical assessment.
Our multidisciplinary and comprehensive diagnostic approach ensures that each patient receives the most appropriate and personalized obesity treatment.
Obesity medications as part of a comprehensive care plan
Pharmacological treatment for obesity should not be understood as an isolated solution, but as part of a structured therapeutic plan.
At barnaclínic+, our approach includes:
1. Comprehensive initial assessment
· BMI calculation and body composition analysis.
· Metabolic and hormonal evaluation.
· Cardiovascular risk assessment.
· Identification of comorbidities.
2. Individualized medication selection
· Clinical profile analysis.
· Selection of the most appropriate molecule.
· Detailed explanation of the mechanism of action.
· Information about realistic expectations.
3. Gradual initiation and dose adjustment
· Progressive dose escalation to minimize side effects.
· Education on medication administration.
· Structured follow-up plan.
4. Ongoing clinical follow-up
· Monitoring of weight and body composition.
· Evaluation of metabolic parameters.
· Therapeutic adjustments if necessary.
5. Maintenance strategy
· Review of treatment goals.
· Continuation plan or modification of therapy.
Why choose a specialized unit for obesity medication treatment?
Choosing where to start pharmacological treatment for obesity is an important medical decision. It is not simply about prescribing a weekly injection, but about managing a complex metabolic disease.
In recent years, the availability of weight-loss medications in non-specialized centers has increased, in some cases without a comprehensive metabolic evaluation or structured follow-up.
At barnaclínic+, pharmacological obesity treatment is based on:

Comprehensive medical assessment
Before initiating any anti-obesity medication, a complete patient evaluation is performed. This allows us to determine the appropriate indication, rule out contraindications and define suitable therapeutic goals.

Selection based on clinical criteria
Not all patients are candidates for the same weight-loss medication. The choice is based on the class of obesity, the presence of diabetes or other associated conditions, and the individual metabolic profile.

Structured follow-up and safe dose adjustment
Treatment requires gradual dose escalation, monitoring of side effects and periodic evaluation. This structured follow-up reduces risks and improves outcomes.

Evidence-based approach
The pharmacological approach is supported by updated clinical protocols and robust scientific evidence, within the healthcare environment linked to the Hospital Clínic of Barcelona.

Beyond weight loss: metabolic and cardiovascular protection
The goal of treatment is not only to reduce body weight, but to improve overall health, lower cardiovascular risk and prevent future complications.
OBESITY EXPERT TEAM
FAQs on Medical Treatment for Obesity
How much weight can be lost with an obesity medication?
Weight loss depends on the patient’s metabolic profile, the class of obesity and the medication used.
New obesity medications have demonstrated significant percentage reductions in body weight in clinical trials when administered under medical supervision.
Beyond the number of kilograms lost, the goal of pharmacological obesity treatment is to improve metabolic control, reduce insulin resistance and lower cardiovascular risk.
What is the cost of an obesity medication?
The cost of an anti-obesity medication depends on the active ingredient, dosage and duration of treatment. Currently, these treatments are not publicly funded for the indication of obesity in Spain.
During the medical consultation, patients receive individualized information about the available options and their estimated cost within the therapeutic plan.
Are obesity medications safe?
Currently approved obesity medications have been evaluated in rigorous clinical trials. However, like any medical treatment, they may cause side effects.
The most common side effects of anti-obesity medications are usually gastrointestinal and generally transient. Medical follow-up allows dose adjustments, monitoring of metabolic parameters and risk minimization.
Use without medical supervision is not recommended.
What are the differences between the various obesity medications?
There are different molecules with specific mechanisms of action. Some act on the GLP-1 receptor, while others have dual action on multiple hormonal pathways involved in metabolism.
The choice of obesity medication depends on the class of obesity, the presence of diabetes or other associated conditions, and individual tolerance.
There is no universal medication suitable for all patients.
How long should obesity medication be taken?
Obesity is a chronic disease. Pharmacological treatment may require medium- or long-term maintenance, always under medical supervision.
Duration depends on the individual response, metabolic evolution and therapeutic goals.
Can I start weight-loss medication without having obesity?
Anti-obesity medications are indicated for patients who meet specific clinical criteria. They are not recommended for purely aesthetic purposes or for individuals without a medical diagnosis of obesity or overweight with comorbidities.
Indication must follow an endocrinological assessment.
What happens if the medication is discontinued?
Obesity is a chronic disease. If treatment is interrupted without a structured follow-up plan, partial weight regain may occur.
For this reason, any adjustment or discontinuation should be medically supervised.
BLOG

Obesity and heart failure: what changes with the new European indication for tirzepatide
March 4, World Obesity Day, is an opportunity to remember that obesity is not an aesthetic issue but a complex chronic disease with a direct impact on metabolic and cardiovascular health. In this context, the recent extension of the European indication for tirzepatide —the active ingredient of Mounjaro— in patients with obesity and heart failure […]
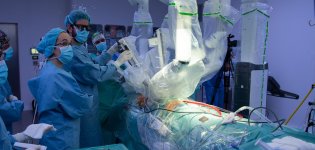
Robotic cardiac surgery at barnaclínic+: a consolidated program with 11 interventions performed in 2025
The robotic cardiac surgery is today one of the most advanced forms of minimally invasive cardiac surgery, making it possible to treat complex heart conditions with the same effectiveness as conventional surgery, but with significantly less surgical trauma. In this context, barnaclínic+ performed 11 robotic cardiac surgeries throughout 2025, integrating this highly complex technique into […]

barnaclínic+ addresses electroporation as a new treatment for atrial fibrillation on the “Salud (t) Plus” podcast
Following the first episode of “Salud (t) Plus”, the barnaclínic+ podcast that launched the format with the real-life experience of Ares Teixidó, who shared how she has learned to live with type 1 diabetes, this new episode focuses on electroporation, an innovative treatment for atrial fibrillation, one of the most common cardiac arrhythmias. Through a […]