13 febrero, 2018
Carcinomatosis peritoneal ¿Qué es y cuál es su tratamiento?
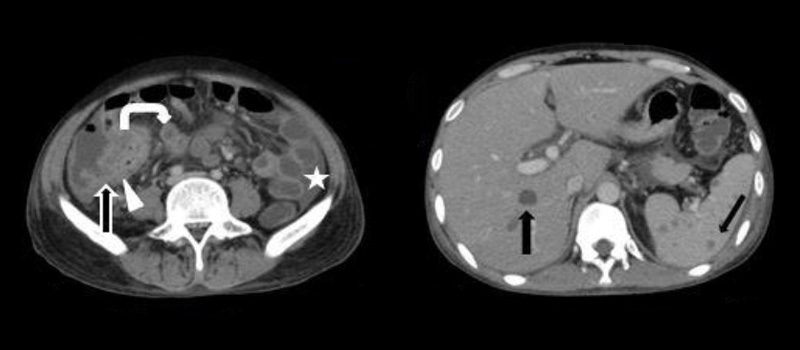
La Carcinomatosis Peritoneal o Carcinosis del Peritoneo (CP) se define por toda diseminación tumoral que afecta de forma localizada o masiva, a la serosa del peritoneo y a los órganos vecinos. De forma mayoritaria puede tener dos orígenes, por un lado, el mismo peritoneo (Pseudomixoma, Mesotelioma) y por otro, un origen en tumores del tracto digestivo o ginecológico.
Tratamiento de la carcinomatosis peritoneal
La realización de técnicas como la Peritonectomía y la Perfusión Hipertérmica de la Cavidad Abdominal han supuesto una revolución en el tratamiento de la Carcinomatosis Peritoneal, antaño considerada una enfermedad terminal. Mediante estos tratamientos, se han conseguido supervivencias mayores al 70% a los 5 años en algunas de estas patologías, con una excelente calidad de vida.
Gracias a los últimos avances en el tratamiento de la carcinomatosis peritoneal conseguimos supervivencias mayores al 70% a los 5 años con una excelente calidad de vida
Así pues, los pacientes afectos de carcinomatosis peritoneal, antaño considerados como terminales y con una esperanza de vida inferior a los 3 meses, pueden disponer en la actualidad de la cirugía cito-reductora (Peritonectomía) y, al finalizar la Peritonectomía, una Perfusión Hipertérmica de la Cavidad Abdominal con fármacos quimioterápicos.
Cirugía cito-reductora o Peritonectomía
La cirguía cito-reductora o Peritonectomía se basa en la extirpación de todo el peritoneo parietal y los nódulos tumorales del peritoneo visceral, en muchas ocasiones con resección de órganos afectados (colon, estómago, bazo, recto).
Perfusión Hipertérmica de la Cavidad Abdominal
La Perfusión Hipertérmica de la Cavidad Abdominal consiste en colocar 4 cánulas en la cavidad abdominal al finalizar la Peritonectomía. Cerrar la cavidad abdominal, conectar las cánulas a una bomba (Performer®) por medio de un circuito de circulación extracorporea.
Con el objetivo de conseguir realizar una hipertermia de la cavidad abdominal (40-41ºC) y administrar durante 60-90 minutos (en función del tipo de tumor) los fármacos quimioterápicos.
Esta técnica de hipertermia se denomina Hipertermia con Abdomen Cerrado, nuestro grupo cree que es una técnica más segura en cuanto a la distribución y acción del fármaco y menos contaminante hacia el personal sanitario, en lugar de la Hipertermia con Abdomen Abierto menos segura en la distribución del fármaco y más contaminante.



mi cuñado le diagnosticaron canser peritonial el tiene 65 años pero a el no le encuetran ningun tumor se hiso exanes como endoscopia escaner ycolodoscopi a
Es una gran esperanza que así sea sin embargo si no es detectado a tiempo, se propaga sin tener un mínimo tratamiento. Es eso o es que en Chile está muy atrasada la medicina. A mi padre lo han desahuciado hoy y cuyo diagnóstico es carcinomatosis peritoneal.
Muy bien la explicación, una luz de esperanza, mi pareja de 48 y 10 meses, cáncer duodeno etapa 4 más drenaje trasparieto hepático., Tiene alguna posibilidad de tratamiento , gracias por alguna respuesta.de antemano. Desde Chile , cuidad de San Fernando.